
Diabetes is a chronic disease that poses a heavy economic burden on the US healthcare system. While diabetes usually does not affect individuals’ ability to do a particular job, the past research has demonstrated that diabetes has great impact on patients, employers and society through reduced productivity at work and at home, work-related absenteeism and health-related work limitations. That’s why, more and more employers are implementing Diabetes Prevention Program (DPP), which is an “evidence-based lifestyle management program to reduce the risk of diabetes among people with prediabetes through improved eating patterns, physical activity, and weight loss”.
DPPs have shown to reduce diabetes and to be cost-effective intervention when used with antidiabetic treatments. The National DPP, recognized by The Centers for Disease Control and Prevention (CDC), provides a framework and brings together partners from the public (federal agencies, state and local health departments, national and community organizations, public insurers) and private (insurers, employers, health care professionals, university community education programs and businesses that focus on wellness) sectors. The DPP can be delivered to adults in the workforce in-person or through virtually. “The economic value of traditional, group-based, in-person DPPs has been demonstrated in cost-effectiveness and health care cost saving studies, with estimates of savings in the range of US$3000+ within 3 years.”. But, what about digital DPPs? Do they perform equally well? Do digital DPPs result in cost savings and health outcomes?
Dr. Castro Sweet and her colleagues tried to answer above questions through their research recently published in the Journal of Health Economics and Outcomes Research (JHEOR). They conducted a longitudinal, observational analysis of health care claims data on a workforce population who received digital DPP and analyzed differences in healthcare utilization and costs from the year prior to program delivery to 1 year after enrollment. The study demonstrated significant short-term health care cost savings at 1 year, driven by reduction in number of hospital admissions and shorter length of stays, among adults in the workforce who participated in digital DPP.
The study reported three key findings:
- Reduction in weight loss
“Among the digital DPP participants, the average weight loss at the end of the intensive phase of the program was 4.3% (SD=5.2%); with 35% of participants achieving at least a 5% weight loss. Weight loss persisted at 4.3% at Week 26, the mid-point of the active treatment year and 2 months into the maintenance phase of the program. This weight loss is similar to that seen in other nationally recognized DPP programs.23 The 12-month weight loss outcome was 3.5%.”
- Medical cost savings
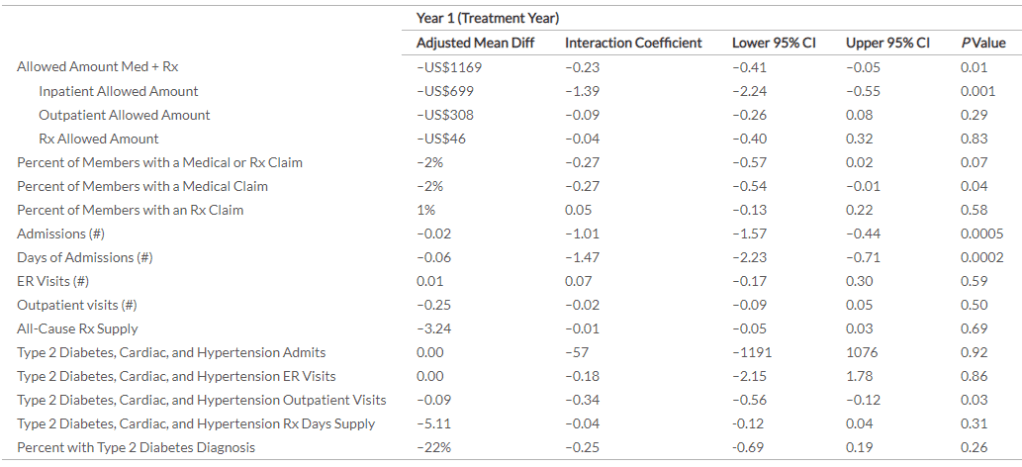
“..in the year after digital DPP enrollment, the digital DPP group had an all-cause, allowed amount of aggregated medical and pharmacy expenditures that were significantly less than the matched comparison group, with an annual cost difference of –US$1169 per participant (P < .05). The savings were primarily from less expenditures for inpatient care (–US$699), with outpatient care (–US$308), and pharmacy (–US$46) contributing to the cost reductions.”
- Reduction in health care utilization
“Consistent with the patterns in expenditures, there was a significantly reduced amount of health care utilization in inpatient care for the digital DPP group in Year 1. Both the average total number of inpatient admissions per person and the length of stay per person were significantly reduced among the digital DPP participants relative to their matched controls.”
Summary: Digital DPP seems to be promising intervention to prevent diabetes and to reduce economic burden on the healthcare system. Importantly, digital delivery of DPP can increase access to the program because it has the ability to reach users at any time or in any location, which is an important consideration during Covid-19 pandemic. Employers and payers should consider improving coverage and uptake of digital delivery of DPP.